|
Treatment with hydrocortisone plus conventional treatment showed better VAS scores at six, 24 and 48 hours when compared with conventional treatment alone and also when compared with placebo. Treatment with gabapentin resulted in better visual analogue scale (VAS) scores after one, two, three and four days when compared with placebo and also when compared with ergotamine plus caffeine at two, three and four days. Treatment with caffeine also decreased the need for a conservative supplementary therapeutic option. Caffeine reduced the number of participants with PDPH at one to two hours when compared to placebo. Two RCTs reported data for PDPH persistence of any severity at follow-up (primary outcome). Pharmacological drugs assessed were oral and intravenous caffeine, subcutaneous sumatriptan, oral gabapentin, oral pregabalin, oral theophylline, intravenous hydrocortisone, intravenous cosyntropin and intramuscular adrenocorticotropic hormone (ACTH). In the original version of this Cochrane review, only seven small RCTs (200 participants) were included. We included 13 small RCTs (479 participants) in this review (at least 274 participants were women, with 118 parturients after a lumbar puncture for regional anaesthesia). These conclusions should be interpreted with caution, due to the lack of information to allow correct appraisal of risk of bias, the small sample sizes of the studies and also their limited generalisability, as nearly half of the participants were postpartum women in their 30s. There is a lack of conclusive evidence for the other drugs assessed (sumatriptan, adrenocorticotropic hormone, pregabalin and cosyntropin). Theophylline has also been shown to increase the proportion of participants that report an improvement in pain scores when compared with conventional treatment. Gabapentin, hydrocortisone and theophylline have been shown to decrease pain severity scores. 
Caffeine has shown effectiveness for treating PDPH, decreasing the proportion of participants with PDPH persistence and those requiring supplementary interventions, when compared with placebo. None of the new included studies have provided additional information to change the conclusions of the last published version of the original Cochrane review. Conclusions should be interpreted with caution. The quality of the studies was difficult to assess due to the lack of information available. No important side effects of these drugs were reported. More people had better pain relief with theophylline (9 in 10 with theophylline compared to 4 in 10 with conventional treatment). Gabapentin, theophylline and hydrocortisone also proved to be effective, relieving pain better than placebo or conventional treatment alone. Caffeine proved to be effective in decreasing the number of people with PDPH and those requiring extra drugs (2 or 3 in 10 with caffeine compared to 9 in 10 with placebo). The trials assessed eight drugs: caffeine, sumatriptan, gabapentin, hydrocortisone, theophylline, adrenocorticotropic hormone, pregabalin and cosyntropin. We included 13 small randomised clinical trials (RCTs), with a total of 479 participants. This is an updated review, and we searched for new trials in July 2014. Lots of drugs are used to treat PDPH, so the aim of this review was to assess the effectiveness of these drugs. 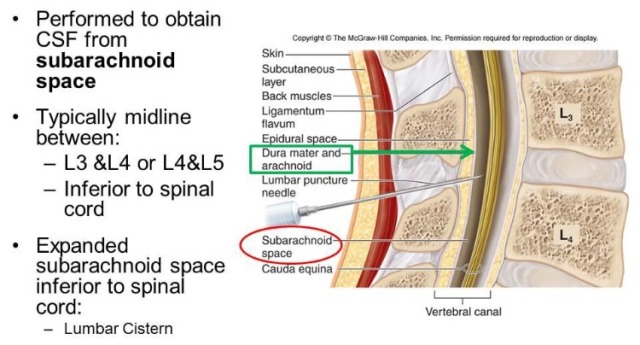
The symptom of PDPH is a constant headache that gets worse when upright and improves when lying down. Post-dural puncture headache (PDPH) is the most common side effect of a lumbar puncture. Although epidural anesthetic is injected just outside the membrane that surrounds the spinal cord, a spinal headache is possible if the membrane is unintentionally punctured.Lumbar puncture involves getting a sample of spinal fluid though a needle inserted into the lower back. Sometimes epidural anesthesia may lead to a spinal headache as well. Spinal headaches typically appear within 48 to 72 hours after a spinal tap or spinal anesthesia. This leakage decreases the pressure exerted by the spinal fluid on the brain and spinal cord, which leads to a headache. Spinal headaches are caused by leakage of spinal fluid through a puncture hole in the membrane (dura mater) that surrounds the spinal cord. 
Tell your health care provider if you develop a headache after a spinal tap or spinal anesthesia - especially if the headache gets worse when you sit up or stand. Spinal headaches are often accompanied by: Pain that typically gets worse when you sit up or stand and decreases or goes away when you lie down.Dull, throbbing pain that varies in intensity from mild to very severe.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
